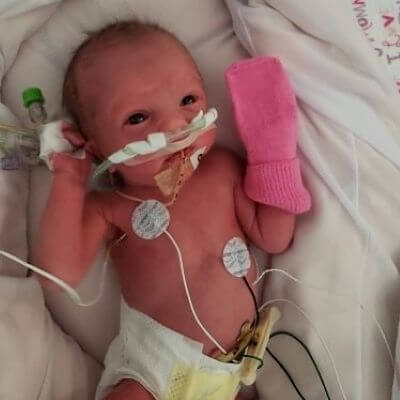
Preemies Run in the Family
Premature birth, also known as preterm birth, occurs in roughly 12% of women in the United States. Any birth before 37 weeks is considered premature. The earlier the delivery, the higher the risk for the baby. Though now, with modern information and technology, babies born as early as 23 weeks and weighing just one pound, one ounce have been successfully saved. Krystina, a patient of Cherokee Women’s Health, was all too familiar with premature birth. Two of her grandparents were born premature, as well as multiple family members. Her own mother was also a preemie. And yes, Krystina herself was born premature. Krystina’s mom delivered her 7 weeks early and almost died in the process. Krystina weighed in at only 3 lbs. 3 ounces. She burst both of her lungs immediately following delivery and spent a couple of months in the NICU (neonatal intensive care). At 11 months old, Krystina only weighed 11 pounds. Preemie Mom Gives Birth to Preemie Babies Fast forward over 30 years and Krystina is a healthy adult who now has had two preemies of her own. Her first baby, her son Augustus, who is now 4 ½ years old, was delivered by Cherokee Women’s Health He was 4 weeks early and delivered via emergency C-section. Her most recent birth of her daughter, Aurelia, happened even earlier. Krystina had a textbook pregnancy with her son up until the last trimester, when she developed high blood pressure. Because of this, she began monitoring her blood pressure at home while pregnant with Aurelia. Once again, all was fine—until the 3rd trimester when her blood pressure started rising again. Developing Preeclampsia Krystina woke up early one morning feeling strangely so she took her blood pressure. It was much higher than before. She called Cherokee Women’s Health, who of course had been monitoring her closely as well, and was told to go to the hospital. Once there, she was diagnosed with preeclampsia (a condition that only occurs during pregnancy, and usually after 20 weeks, and can be very dangerous for the mom and baby. High blood pressure is one of the signs). It was decided that she should be admitted but the hospital’s NICU was full, so she was transferred to a different hospital in anticipation of the baby coming early. The next 9 days were very hard on Krystina. She was in a hospital further from home, she hadn’t gotten to say goodbye to her son, and she was very worried about her new baby making an early entrance. Thankfully, the doctors were able to stabilize her blood pressure and after a few days, she was sent back to her local hospital. But once there, her blood pressure elevated again so the decision was made to deliver her baby. Going Home Without Her Baby Her doctor of Cherokee Women’s Health performed a C-section and Aurelia was born 7 weeks early and weighed only 3 lbs. 8 oz., just 5 ounces more than Krystina had weighed when she was born. Aurelia spent the next 13 days in the NICU due to needing oxygen and being a little jaundiced. Overall though, she was strong and doing well. Krystina was also doing well and was released after 2 days. Going home without her baby was one of the hardest things she has ever done. Baby is Home and Healthy! Today Aurelia is a beautiful and healthy 10-month-old daddy’s girl. She is a great eater and has quickly grown to almost 20 pounds. “My doctors played such a crucial role in making sure my babies were fine. They are both fantastic. Their calm demeanors and support really helped me to relax.” – Krystina shares about her experience at Cherokee Women’s Health Krystina and her husband are so grateful that both of their preemies are doing so well. Those babies, and Krystina herself, are great examples of how premature babies can go on to live happy, healthy lives.