
At just 32 years old, a uterine prolapse was the last thing Laurie expected.
After all, everything had been going great for Laurie and her husband Christopher. Even though they had suffered from a devastating miscarriage at 10-1/2 weeks – after nine months of trying – they tried again, and were blessed with a beautiful, healthy baby boy.
Feeling – and Seeing – Something Strange Down There
During a workout one evening, Laurie felt a strange pressure between her legs, sort of a tugging feeling. She wasn’t quite sure what it was, but she knew something wasn’t right.
Later while washing herself in the shower she felt — and saw — a visible bulge. Laurie freaked out! She had no idea what was happening, or if this was something dangerous. After talking to her husband, they knew she needed to see her doctor.
Consulting with Dr. Haley
She had known Dr. James Haley for years and had trusted him with many of her GYN issues. She knew his expert advice would be valuable, since he was not only an OB/GYN, but also a double board-certified urogynecologist. She made an appointment with her doctor right away.
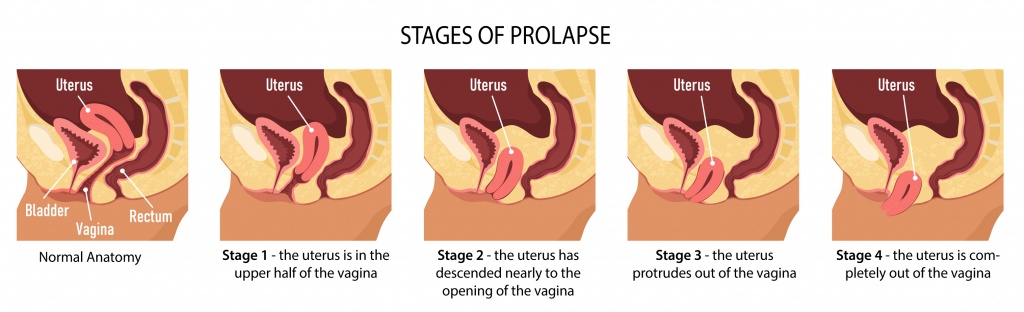
During her exam, it was discovered that Laurie had a stage 3 uterine prolapse. A stage 3 uterine prolapse is when the uterus drops down and protrudes out of the vagina. Laurie was confused and scared. Her doctor explained that while not dangerous or life-threatening, prolapse can cause pain and discomfort, and may make some desired activities difficult or impossible. It was also explained to her that if left untreated, it would stay the same or progressively get worse.
‘Worse’, Laurie thought, ‘what could be worse than a part of your body protruding out of your vagina?’ Her doctor told her it could lead to problems with incontinence, cause discomfort during sex, and lead to complications in another pregnancy, among other things.
Stage 3 Uterine Prolapse – How Did This Happen?
Laurie wondered what could have caused this to happen. There can be numerous causes such as:
- Having one or more babies come through the birth canal
- Obesity
- Activities involving a lot of heavy lifting and straining
- Age
- Smoking, and other factors.
All in the Family
Pelvic organ prolapse can also be a hereditary disorder, meaning that it runs in families. Since our genes influence the strength of our bones, muscles, and connective tissue, some women are born with weaker tissues and are a higher risk for prolapse.
After talking to her mom, Laurie discovered that she had a prolapse and a hysterectomy before she was 30 years old. Laurie had no idea! She also learned that all of her mom’s sisters experienced pelvic organ prolapse as well.
Prolapse Solutions
Laurie knew she had to learn what could be done to correct it, regardless of the cause. Her doctor told her that pelvic floor exercises can improve the symptoms in mild and moderate cases (first- to second-degree prolapse), and sometimes also prevent the organs from slipping down further. But in Laurie’s case, her prolapse was too far gone.
Her doctor then explained that in cases as severe as hers, a hysterectomy is often needed to correct prolapse. Laurie knew she and Christopher wanted more children, so she didn’t even want to discuss that option, so her doctor suggested using a pessary.
A Pessary Helps Hold the Uterus Up
A pessary is a soft, removable device that can be inserted into the vagina to support its internal structure. Basically, it would help to hold her uterus up, back where it belonged. Her doctor would insert it and she would come back for follow-up visits to remove it and make sure all was going well. There are very few side effects with the use of a pessary, and they are usually alleviated by just removing it.
Laurie went home that day feeling informed and hopeful. She discussed her options with Christopher, and they decided she should give the pessary a try. She thought, ‘Who knows, maybe the pessary would help the uterus stay where it belonged, even after she removed the device.’ That was not the case.
The Pessary Worked for Years, But Wasn’t Ideal for Laurie
The next few years went by with Laurie using the pessary and having it changed as needed. It wasn’t that it hurt, but she could often feel it during intercourse and while exercising. Not ideal. She and Christopher had discussed getting pregnant again but after a GYN appointment, it was affirmed that her prolapse was not any better and had actually gotten a little worse. Her doctor also informed her that the pessary would need to come out if she got pregnant and that, with the weight of a baby in her uterus, there was a big possibility she could spend much of her pregnancy on bedrest. Laurie had a full-time job, as well as a 3 ½ -year-old at home, so this was not an option for her.
Making a Difficult Decision
After lots of praying, discussing, and researching — and finally at 37 years old — Laurie and Christopher made the very difficult decision for her to have a hysterectomy. This was one of the toughest decisions Laurie ever had to make.
Laurie underwent a partial hysterectomy, vaginally, removing her uterus only. After six weeks, she was feeling back to normal, physically that is, but emotionally still feeling the loss of not being able to have any more children. She and Christopher felt very blessed though, they did have a healthy and active, 5-year-old.
Thankful for Dr. Haley’s Expertise and Compassion
Laurie was very thankful for the expertise and compassion of her doctor through the whole journey.
“Dr. James Haley had been helping me with my OB/GYN issues for many years. So, when I needed an expert, I knew I could trust him. Dr. Haley helped me get my life back on track and guided me along my journey.”
– Laurie
While her case was severe, not all prolapses result in a hysterectomy. Some can be corrected with other treatments.
Laurie offers this advice for other women, “Make sure to find a qualified expert who you can trust and who has lots of experience. Don’t be embarrassed to discuss anything going on with your body. Your doctor has seen it all and can guide you to the right decision for you”.


