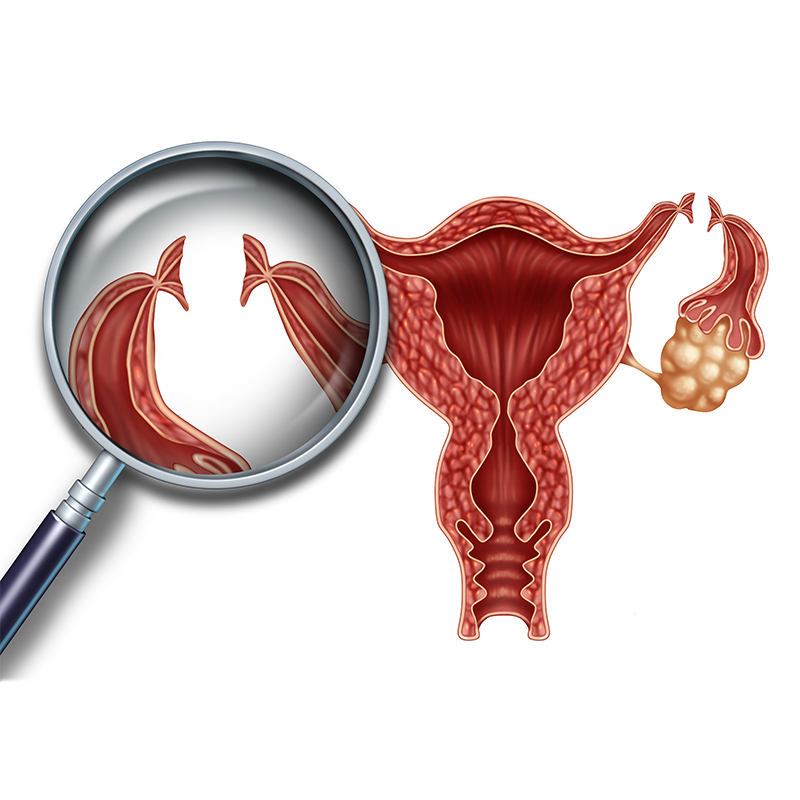
Tubal Ligation: When Should I Get my Tubes Tied?
Commonly referred to as “getting your tubes tied,” tubal ligation is a permanent surgical procedure that is performed to prevent pregnancy. More formally, it’s also known as female sterilization. In recent years, the term “tubal sterilization” is most accurate, since the technical definition of the word “ligation” refers to a specific surgical technique that is no longer used in most sterilization surgeries. Whatever the term you prefer, the procedure involves closing off a woman’s fallopian tubes to prevent eggs from traveling down to the uterus, and prevents pregnancy. When Can Tubal Ligation be Performed? Tubal ligation can be done in conjunction with childbirth, since the advantage is that it can be performed at the same time as a C-section or within 48 hours of a vaginal delivery. Many surgeons prefer to do the surgery after birth because you’re already in the hospital, and your abdominal muscles are still relaxed from having just given birth. If you decide later on that a tubal sterilization is the procedure for you, it can also be done as an outpatient procedure separate from childbirth via interval tubal ligation. This process uses a laparoscope, a thin tube with a camera lens and light on the end. The procedure involves general anesthesia to prevent any pain or discomfort. What to Expect During the Procedure If you have an interval tubal ligation as an outpatient procedure, either a needle is inserted or an incision is made through your navel so your abdomen can be inflated with gas (carbon dioxide or nitrous oxide). Then the laparoscope is inserted into your abdomen. In most cases, your doctor will make a second small incision to insert special instruments. Using these instruments passed through the abdominal wall, your doctor seals the fallopian tubes by destroying segments of the tubes or blocking them with plastic rings or clips. If you have a tubal ligation after vaginal childbirth, your doctor will likely make a small incision under your navel, providing easy access to your still-enlarged uterus and fallopian tubes. If you have a tubal ligation during a C-section, your healthcare provider will use the same incision that was made to deliver the baby. What to Expect After a Tubal Ligation Procedure If your abdomen was inflated with gas during the interval tubal procedure, the gas will be withdrawn. You may be allowed to go home several hours after the procedure. If you have the procedure in combination with childbirth, the tubal ligation isn’t likely to add to your hospital stay. You may have some discomfort at the incision site afterwards. Other symptoms you may experience include: Abdominal pain or cramping Fatigue Dizziness Gassiness or bloating Shoulder pain You may take acetaminophen (e.g. Tylenol) or ibuprofen (Advil, Motrin IB, others) for pain relief, but avoid using aspirin, since it may increase bleeding. Your doctor will most likely permit you showering or bathing 48 hours after the procedure, but will advise against straining or rubbing the incision for a week. You should also avoid strenuous lifting and sex for one to two weeks, but can resume your day-to-day activities gradually as you begin to feel better. Your stitches will dissolve and won’t require removal. If you have any concerns that you aren’t healing properly, it’s important to call your doctor to see if you need a follow-up appointment. Additionally, contact your health care provider immediately if you experience: A temperature of 100.4 F (38 C) or greater Fainting spells Severe abdominal pain that’s persistent or gets worse after 12 hours Bleeding from your incision that’s persistent or gets worse after 12 hours, despite use of pressure and bandages Discharge from your incision that’s persistent or gets worse. Who is the Ideal Candidate for Tubal Ligation? Tubal sterilization is considered a permanent surgery, so it’s a good option only if you’re completely sure you don’t want any more children. If you’re not entirely sure if you’re done having children, you might consider other less permanent forms of birth control. While you may have heard of women who successfully get their tubal sterilizations reversed, it isn’t guaranteed to be effective, and involves a second invasive surgery. Additionally, because tubal sterilization is a surgery, your doctor may advise against the surgery if you’re obese, have chronic health conditions such as heart disease, or if you’ve had complicated abdominal surgeries in the past. Complications If you think you may be pregnant after your tubal ligation procedure, you should contact your health care provider immediately. While tubal ligation is highly effective in preventing most pregnancies, it isn’t an absolute in preventing pregnancy. An estimated 1 out of every 200 women will become pregnant after tubal ligation. Complications related to tubal ligation include an increased risk of an ectopic pregnancy, which happens when a fertilized egg implants in the fallopian tubes instead of traveling to the uterus. An ectopic pregnancy can be dangerous, and can cause a rupture in the fallopian tube, resulting in internal bleeding. Contact Us In 95% of cases, tubal ligation is an effective permanent form of birth control. Before deciding if this procedure is the best fit for you, it’s important to consider all the possibilities and know your options. If you think tubal ligation might be the right permanent birth control option for you, we invite you to call us at 770.720.7733 or schedule an appointment online with one of our board-certified obstetricians.